Zombies: A Scientific and Psychological Approach
Written by Kevin Volkan and Neil Rocklin
Originally published in Bizarre Behavior blog on September 28, 2011. Special thanks to Kevin for allowing us to repost!
 Recently I ran across some articles that got me thinking of ‘zombification’ in the animal Kingdom. A really great summary by Mo Constandi on his blog Neurophilosophy (Costandi, 2006) as well as an article by Evans, Elliot, & Hughes (2011) describe brain altering fungi – usually from the genusCordyceps. This entomopathogen(something that causes disease in insects) infects ants when its spores attach to the outside of the insect. The spores then germinate growing into the interior of the ant’s body through the spiracles (i.e. respiratory holes in the exoskeleton) or its trachea (or throat). The fungus then sends mycelia, which are filament-like roots, into the body of the ant where it feeds on any soft tissue while avoiding any organs necessary for the ant’s survival. Eventually, the mycelia grow into the ant’s nervous system where they release chemicals that affect its brain. This causes the ant to change its behavior. Typically, the ant will then climb up a plant to an exposed location where it will then clamp on to a leaf. At this point the fungus will then consume the ant from the inside out and produce spores. These fruiting bodies (i.e. the ‘mushroom’ part of the fungus) will then sprout from the ant’s head and body. The fungus will then release spores from the fruiting body and exposed location of the ant will allow these spores to spread via the air and hence to other ants.
Recently I ran across some articles that got me thinking of ‘zombification’ in the animal Kingdom. A really great summary by Mo Constandi on his blog Neurophilosophy (Costandi, 2006) as well as an article by Evans, Elliot, & Hughes (2011) describe brain altering fungi – usually from the genusCordyceps. This entomopathogen(something that causes disease in insects) infects ants when its spores attach to the outside of the insect. The spores then germinate growing into the interior of the ant’s body through the spiracles (i.e. respiratory holes in the exoskeleton) or its trachea (or throat). The fungus then sends mycelia, which are filament-like roots, into the body of the ant where it feeds on any soft tissue while avoiding any organs necessary for the ant’s survival. Eventually, the mycelia grow into the ant’s nervous system where they release chemicals that affect its brain. This causes the ant to change its behavior. Typically, the ant will then climb up a plant to an exposed location where it will then clamp on to a leaf. At this point the fungus will then consume the ant from the inside out and produce spores. These fruiting bodies (i.e. the ‘mushroom’ part of the fungus) will then sprout from the ant’s head and body. The fungus will then release spores from the fruiting body and exposed location of the ant will allow these spores to spread via the air and hence to other ants.

Ant with Cordyceps Fruiting Body Growing from its Brain
Such a relationship between parasites and insects is not unusual and there are many other examples in the animal kingdom. For instance a similar example involves crickets that are infected bynemotodes (roundworms) that cause them to jump into water facilitating the nematode lifecycle (Thomas et al., 2003). Lewis (1974) describes the life cycle of Leucochloridium helminthes (worms), which infect terrestrial mollusks (snails). The worms infect the snails and form broodsacs in the snail’s tentacles. The tentacles become striated, swell, and pulsate mimicking something like a maggot – a favorite food for birds. The worm also changes the snail’s behavior so that it moves to an exposed place. Birds are attracted to the maggot-like tentacles and bite them off the snails. The worm larvae are then excreted by the bird ready to infect another snail. The snails do not necessarily die, the tentacles can regenerate, and more broodsacs can be formed.* Other snails infected with helminthes may instead be castrated by the broodsac that form inside the snail.

Snail with Leucochloridium Infection
The phenomena of parasites changing the behavior of a host are not limited to insects and mollusks. There is evidence that infection by the intracellular protozoa Toxoplasma gondii changes the behavior of rats. Rather than showing aversion to cats the rats no longer act as if the cats are no longer predators and in some instances are attracted to them. This of course results in the infected rats being eaten and the cats facilitating the life cycle of the parasite through harboring the protozoa and then excreting it in their feces.
 T. gondii is infectious to all mammals and will infect the human nervous system in particular. Pregnant women infected with T. gondii can pass it on to their unborn children causing serious problems such as cerebral palsy, mental retardation, and even death. This is why pregnant women should not change the kitty litter!
T. gondii is infectious to all mammals and will infect the human nervous system in particular. Pregnant women infected with T. gondii can pass it on to their unborn children causing serious problems such as cerebral palsy, mental retardation, and even death. This is why pregnant women should not change the kitty litter!
Generally infection with T. gondii is asymptomatic in the initial stages though it has been linked to psychotic symptoms in humans, especially those who have compromised immune systems. Late stage T. gondii infection has been linked to personality changes, a decrease in intelligence, psychomotor performance degradation, certain types of brain tumors, and schizophrenia. A paper by Webster et. al. (2006) clearly outlines the evidence for the association of T. gondii infection and schizophrenia. The authors hypothesize that anti psychotic medications such as haloperidol may work in part because they have anti – T. gondii properties. In fact, the authors found that haloperidol and valproic acid were as effective in controlling T. gondii infection in rats as standard anti – T. gondii medications. The authors conclude that their findings could “lead to improved prognosis and potentially new medication combinations and therapeutic modalities for the treatment of both toxoplasmosis and severe psychiatric disorders” (p. 1029). Seen from this light it is possible that schizophrenia associated with T. gondii infection could be seen as a form of ‘zombie-ism’ – one that could be treated by eradicating the protozoa, which is also be a potentially new way of dealing with psychosis!
Of course humans suffer from other types of nervous system infections that could potentially affect behavior. For example one of the most common and oldest known infection of the brain is caused by Taenia solium otherwise known as the tapeworm. T. solium usually enters the body when a person eats undercooked pork that carries the eggs of the tapeworm. These hatch in the intestines and live in this ‘food rich’ environment. But sometimes T. soliummakes its way into the bloodstream where it can travel to the muscles, eyes, or brain.
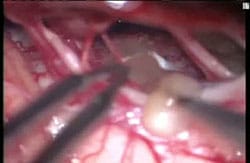
Live Tapeworm being Removed from a Human Brain
In 2008 Fox news reported on a woman in Arizona who had a live tapeworm in her brain (“It’s Not a Tumor – Doctors Find Worm In Woman’s Brain Instead,” 2008). She had reported numbness in her arm and blurred vision and doctors suspected a tumor. Indeed something showed up on a MRI scan and the woman was scheduled for surgery. During the operation for an expected tumor the woman’s surgeon found the live worm and removed it.** Interestingly, this woman was lucky because once the worm was removed her neurological symptoms resolved. Worse problems may arise if the worm dies while in the brain. When this happens an inflammatory immune action is provoked and a cyst is formed around the worm. This can cause headaches, encephalitis, seizures, and in some cases zombie-like mental confusion as well loss of coordination and balance. While single cyst-caused lesions are less problematic, people who have multiple or calcified lesions may have permanent neurological issues (Singhi, 2011). T. solium infection highlights the importance of fully cooking food like pork as well as the necessity for good hygiene among those who handle food.
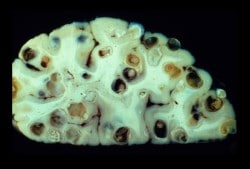
Neurocysticercosis – Tapeworm Cysts in the Brain
The infections cited above, whether deliberately part of an organism’s life cycle (as with Cordyceps orLeucochloridium) or accidental (as with T. gondii or T. solium), cause damage to the brain. There are of course other pathogens such as viruses that can also infect the brain. These infections result inencephalitis, which is an inflammatory response causing swelling and irritation that are potentially life threatening. Encephalitis is most often caused by a virus and usually results in mild flu-like symptoms. However, encephalitis is unpredictable. Severe cases can be deadly or cause permanent brain damage, having at least the potential to create a zombie-like state. Some pathogens, like viruses in the Herpes simplex (HSV) group can cause severe encephalitis.
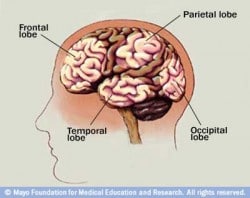
Three of the HSV types (HSV-1, HSV-2, and Varicella zoster) can infect the human nervous system. HSV-1 (commonly known as oral herpes) is the most common cause of viral encephalitis that can be life threatening. HSV-1 has a preference for infecting the frontal cortices, which can produce a number of neurological problems, including language and memory impairment as well as epilepsy. Psychological issues such as personality and behavioral abnormalities, including disinhibition and increased aggression can also occur (Arciniegas & Anderson, 2004). HSV-2 (the type responsible for genital herpes) infection can also produce encephalitis that causes neuropsychological symptoms. While HSV-2 seems to have a preference for infecting the meninges (tissues around the brain), it can also affect the brain, brainstem, cranial nerves, nerve roots, and spinal cord, as well. This can result in cranial nerve damage (neuropathy), weakening (hemiparesis) or loss of sensation (hemisensory loss) on one side of the body, and altered levels of consciousness. Typical herpes skin lesions may accompany neurological infection (Berger, Houff, & Fathallah-Shaykh, 2008). It seems plausible that people suffering from untreated neurological HSV 1 & 2 encephalitis could look and behave like zombies.

Heinrich Kluver
Another serious possible consequence of HSV encephalitis is Kluver-Bucy Syndrome (KBS) (Begum, Nayek, & Khuntdar, 2006; Cohen, Park, Kim, & Pillai, 2010; D Ku & Sang Yoon, 2011; Duggal, Jain, Sinha, & Nizamie, 2000; Gabison-Hermann, Pelletier, Taleb, & Bouleau, 2009; Yilmaz et al., 2008). Heinrich Kluver was a German émigré experimental neuropsychologist at the University of Chicago. He served as a German soldier from World War I and was wounded. A trip to the base hospital spared him from defending against the final Allied assault and perhaps saved his life. Those who didn’t know him well found him diffident and somewhat perfectionistic – almost a cliché of German scientists from this era. His friends however know him as a warm and thoughtful scientist. Kluver studied eidetic imagery, which led him to study hallucinations induced through mescaline. Reportedly Kluver used himself as a guinea pig with regard to the effects of mescaline and an overdose supposedly left him seriously ill for a time. After studying the effects of mescaline on monkeys he began experiments with neurosurgeon Paul Bucy on the effect of removing the temporal lobes of the brain in their primate subjects. The loss of the temporal lobes produced a syndrome that was named after the two researchers. (Hunt, 1980).

Paul Bucy
Kluver-Bucy Syndrome (KSB) results in marked behavioral changes which include hyperorality (putting things in the mouth), hypoermetamorphosis (a fixation of attention to something in the environment – usually related to orality), hypersexuality, and a supposed passive ‘tameness’ (Klüver & Bucy, 1937, 1938, 1939). The last quality has been construed as a lack of aggression in that caged monkeys with KBS were more placid and easily approached. However, in a later experiment by Kling where the monkeys were allowed to roam freely after the operation, it was noted that the animals did not act tame and were not easily approached, but instead became socially isolated (Glick & Roose, 1993).
In humans KBS results in behavioral changes similar to those in monkeys. These changes, however, are more elaborate and include amnesia, Attention-Deficit/Hyperactivity Disorder, confusion, aggression and frustrated rage, pica (eating non-edible things including corprophagia), dysphasia (impairment in speech and comprehension of speech), emotional blunting and lability, hypermetamorphosis, hyperorality (which in one case involved continual spitting), hypersexuality, impulsivity, passivity, visual agnosia (inability to make sense of what is seen), etc. (Begum et al., 2006; Berger et al., 2008; Cohen et al., 2010; D Ku & Sang Yoon, 2011; Duggal et al., 2000; Gabison-Hermann et al., 2009; Greenwood, Bhalla, Gordon, & Roberts, 1983; Lilly, Cummings, Benson, & Frankel, 1983; Yilmaz et al., 2008). There can be a number of causes of KSB in humans (besides encephalitis) and damage to the temporal lobes may vary to a great degree (Lilly et al., 1983). Interestingly the studies of KSB in humans often report some form of aggression. Clearly many of the aspects of KSB listed above could be seen as indicative of a form of ‘zombie-ism’.
 I am familiar with KSB from my psychological practice at a large state mental hospital. When I worked in a skilled nursing ward I had a patient (who I will call) John who demonstrated many aspects of KSB in humans.
I am familiar with KSB from my psychological practice at a large state mental hospital. When I worked in a skilled nursing ward I had a patient (who I will call) John who demonstrated many aspects of KSB in humans.
John’s life was a tragedy. At age five he was playing in his driveway behind his parent’s car. His father, rushing off to work, failed to notice the little boy and backed the car up, driving over the boy’s head. John survived but suffered severe brain injury on one side to his temporal and frontal lobes. He became developmentally delayed (what used to be called ‘retarded’) and his behavior became unruly and violent. John’s behavior became so bad his parents couldn’t handle him at home and he was committed to a state mental institution. When I began to work with John he was 30 years old and had grown up in the mental hospital. This was not a good place to grow up. In John’s case being an unruly violent child in the company of other unruly violent children meant constant fights and injuries. When John became a teenager he got in an especially bad fight that resulted in his head being repeatedly smashed against a concrete floor by an older, much stronger patient. This patient had no idea of what he was doing and kept hitting John’s head against the floor until John almost died.
John suffered further traumatic brain injury from this incident, this time to the temporal and frontal lobes on the other side. Whereas after the first injury John could talk and reason to some degree, after second he could not. His demeanor was that of being in a awakened vegetative state. John also suffered damage to his motor cortex and was paralyzed from the waist down. More interestingly though (and the point of this story) is that the damage to John’s frontal lobes resulted in KBS. In essence, John became an eating machine. Without consciousness John would spend every waking second trying to eat something, whatever came within his grasp. He would constantly pick at his clothes until he could rip off chunks and eat them. John’s physician showed me an old X-ray of John’s stomach which was filled with cloth, a couple of forks, toys, anything he could fit in his mouth.
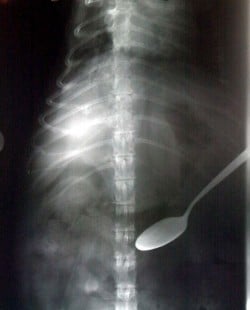
X-Ray of the Stomach of a Person With Pica Behavior
John would also try and eat people. When you came close to John he would reach out, grab you, and try to get a bite. Because of this insatiable appetite for anything he could get his hands on, John spent his days dressed in rip-stop clothing, with his arms tied down in restraints. This drive to eat had no conscious motivation to it, and John exhibited no consciousness at all – eating was the whole of John’s being. John exhibited hypermetamorphosis in that once he locked on to something in the environment he would focus obsessively on trying to eat it. John was not usually aggressive, except if he were kept from something he wanted to eat. Then he would become frustrated and somewhat enraged. Had John able to walk, he would certainly have attacked people and tried to eat them. He had in essence become a zombie.
For me, the case of John and others like him brings up the real possibility of zombie-ism. The one saving grace in this nightmare scenario is that fully mobile and unrestrained, John-like zombies would soon eat themselves to death. They could not keep ingesting inedible objects without serious consequences. Unless John-like zombies somehow developed a taste for living creatures, the rest of us wouldn’t have much to worry about and after a few days of unrestrained eating they would either be debilitated or dead. All enterprising survivors would have to do would be to hole up somewhere and wait out the ‘zombacolypse’.
Yet the case of John and others like him give hard evidence that an infectious agent or trauma can cause injury to the brain leading to zombie-like behavior changes. This scenario is far-fetched perhaps, but not impossible. Harvard psychiatrist Steven Schlozman elaborates on this idea in his book The Zombie Autopsies: Secret Notebooks from the Apocalypse (Schlozman, 2011). In this fictional account an infectious agent has caused a pandemic. The infection itself is man-made comprising a virus that delivers prion disease to the brain, selectively destroying its higher centers. The virus/prion combination (and a third infectious agent the protagonists try to identify) also infect the body, leaving just enough function to allow the zombie to move and eat. I would suggest that in real life such an elaborate mechanism is not necessary. There are plenty of prospects in the world at large that have the potential to be ‘zombifying’ agents. A small mutation in one of theherpes viruses or T. gondii, a tapeworm variant, a fungus that jumps from insects to humans, or some combination thereof could do the trick. Given these infectious agents our obsession with zombies starts to makes sense. Perhaps in the back of our minds we realize there is the possibility of a real zombie outbreak, that there is something to be afraid of?
Notes
* There is a wonderful video of these snails online at http://youtu.be/EWB_COSUXMw
** Video of the worm being removed can be found here: http://media2.foxnews.com/112008/worm_tumor_700.wmv
References
Arciniegas, D. B., & Anderson, C. A. (2004). Viral encephalitis: Neuropsychiatric and neurobehavioral aspects. Current Psychiatry Reports, 6, 372-379. doi:10.1007/s11920-004-0024-x
Begum, H., Nayek, K., & Khuntdar, B. K. (2006). Kluver-Bucy syndrome–a rare complication of herpes simplex encephalitis. Journal of the Indian Medical Association, 104(11), 637-638.
Berger, J. R., Houff, S., & Fathallah-Shaykh, H. M. (Ed. . (2008). Neurological complications of herpes simplex virus type 2 infection. Archives of Neurology, 65(5), 596-600. doi:10.1001/archneur.65.5.596
Cohen, M. J., Park, Y. D., Kim, H., & Pillai, J. J. (2010). Long-term neuropsychological follow-up of a child with Klüver–Bucy syndrome. Epilepsy & Behavior, 19(4), 643-646. doi:10.1016/j.yebeh.2010.09.003
Costandi, M. (2006, November). Brainwashed by a parasite «?Neurophilosophy. Retrieved September 14, 2011, from http://neurophilosophy.wordpress.com/2006/11/20/brainwashed-by-a-parasite/
D Ku, B., & Sang Yoon, S. (2011). Relapsing herpes simplex encephalitis resulting in Kluver-Bucy syndrome. Internal Medicine (Tokyo, Japan), 50(7), 763-766.
Duggal, H. S., Jain, R., Sinha, V. K., & Nizamie, S. H. (2000). Post-encephalitic Kluver-Bucy syndrome. Indian Journal of Pediatrics, 67(1), 74-76.
Evans, H. C., Elliot, S. L., & Hughes, D. P. (2011). Hidden diversity behind the zombie-ant fungus Ophiocordyceps unilateralis: four new species described from carpenter ants in Minas Gerais, Brazil. PloS One, 6(3), e17024. doi:10.1371/journal.pone.0017024
Gabison-Hermann, D., Pelletier, A., Taleb, M., & Bouleau, J.-H. (2009). [The case of temporal lobes dysfunction in atypical psychiatric episodes]. L’Encéphale, 35(5), 491-495. doi:10.1016/j.encep.2008.06.013
Glick, R. A., & Roose, S. P. (1993). Rage, power, and aggression. Yale University Press.
Greenwood, R., Bhalla, A., Gordon, A., & Roberts, J. (1983). Behaviour disturbances during recovery from herpes simplex encephalitis. Journal of Neurology, Neurosurgery, and Psychiatry, 46(9), 809-817.
Hunt, W. A. (1980). Heinrich Klüver: 1897-1979. The American Journal of Psychology, 93(1), 159-161.
It’s Not a Tumor – Doctors Find Worm In Woman’s Brain Instead. (2008, November 20). Text.Article, . Retrieved September 27, 2011, from http://www.foxnews.com/story/0,2933,455067,00.html
Klüver, H., & Bucy, P. C. (1937). “Psychic blindness” and other symptoms following bilateral temporal lobectomy in Rhesus monkeys. American Journal of Physiology, 119, 352-353.
Klüver, H., & Bucy, P. C. (1938). An analysis of certain effects of bilateral temporal lobectomy in the rhesus monkey, with special reference to “psychic blindness.” Journal of Psychology: Interdisciplinary and Applied, 5, 33-54.
Klüver, H., & Bucy, P. C. (1939). Preliminary analysis of functions of the temporal lobes in monkeys. Archives of Neurology & Psychiatry (Chicago), 42, 979-1000.
Lewis, P. D. (1974). Helminths of Terrestrial Molluscs in Nebraska. II. Life Cycle of Leucochloridium variae McIntosh, 1932 (Digenea: Leucochloridiidae). The Journal of Parasitology, 60(2), 251-255. doi:10.2307/3278459
Lilly, R., Cummings, J. L., Benson, D. F., & Frankel, M. (1983). The human Klüver-Bucy syndrome. Neurology, 33(9), 1141-1145.
Schlozman, S. C. (2011). The Zombie Autopsies: Secret Notebooks from the Apocalypse. Grand Central Publishing.
Singhi, P. (2011). Neurocysticercosis. Therapeutic Advances in Neurological Disorders, 4(2), 67-81. doi:10.1177/1756285610395654
Thomas, F., Ulitsky, P., Augier, R., Dusticier, N., Samuel, D., Strambi, C., Biron, D. ., et al. (2003). Biochemical and histological changes in the brain of the cricket Nemobius sylvestris infected by the manipulative parasite Paragordius tricuspidatus (Nematomorpha). International Journal for Parasitology, 33, 435-443.
Webster, J. P., Lamberton, P. H. L., Donnelly, C. A., & Torrey, E. F. (2006). Parasites as Causative Agents of Human Affective Disorders? The Impact of Anti-Psychotic, Mood-Stabilizer and Anti-Parasite Medication on Toxoplasma gondii’s Ability to Alter Host Behaviour. Proceedings: Biological Sciences, 273(1589), 1023-1030.
Yilmaz, C., Cemek, F., Güven, A. S., Caksen, H., Ata?, B., & Tuncer, O. (2008). A child with incomplete Kluver-Bucy syndrome developed during acute encephalitis. The Journal of Emergency Medicine, 35(2), 210-211. doi:10.1016/j.jemermed.2007.05.051



